Mpox, formerly known as Monkeypox, is a rare viral disease that has gained global attention. It is now a larger concern as on the 15th of August 2024, the World Health Organisation (WHO) declared Mpox a public health emergency of international concern due to a new variant being found in several African countries. We aim to educate South Africans about Mpox, its transmission, symptoms, and prevention strategies to help control its spread and ensure public health safety.
What is Mpox?
Mpox is caused by the monkeypox virus, a member of the Orthopoxvirus genus, which also includes the variola virus (causing smallpox). There are currently more than 80 poxviruses known to science which have been isolated from different species of birds, insects, reptiles, marsupials and mammals.
These zoonotic viruses are harboured by different animal species and may spill over to the human population when there is sufficient exposure. First discovered in 1958 in laboratory monkeys, Mpox was identified in humans in 1970 in the Democratic Republic of Congo. Unlike smallpox, which was eradicated globally in 1980, Mpox continues to occur in certain parts of Africa, notably in Central and West Africa as it is endemic in densely forested regions.
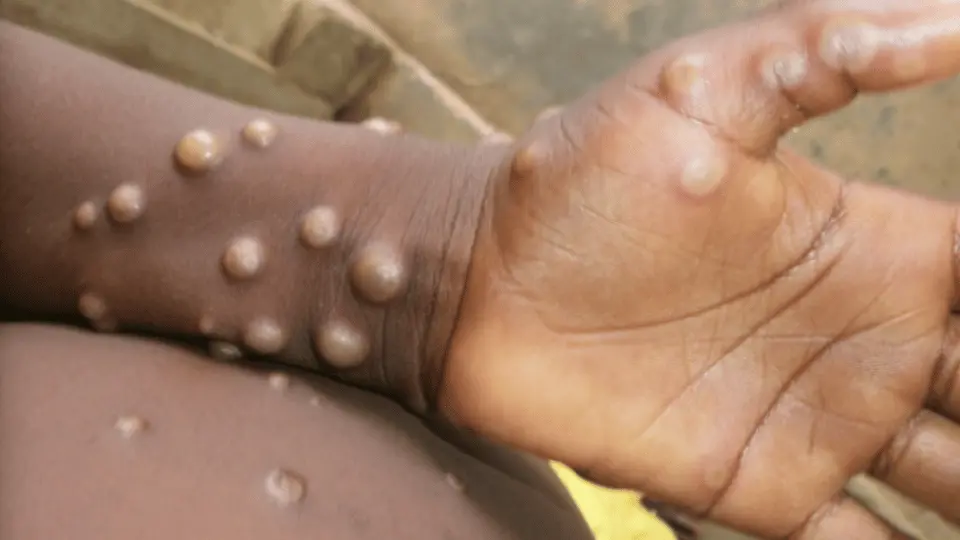
Mpox in Context
It is helpful to compare Mpox with other infectious diseases to understand it in a broader context. Unlike COVID-19, which spreads primarily through respiratory droplets, Mpox requires closer contact for transmission. Historical outbreaks of Mpox in Central and West Africa provide valuable lessons on containment and prevention strategies. The current outbreak in South Africa highlights the need for vigilance and preparedness to manage emerging infectious diseases.
Mpox Outbreak in South Africa
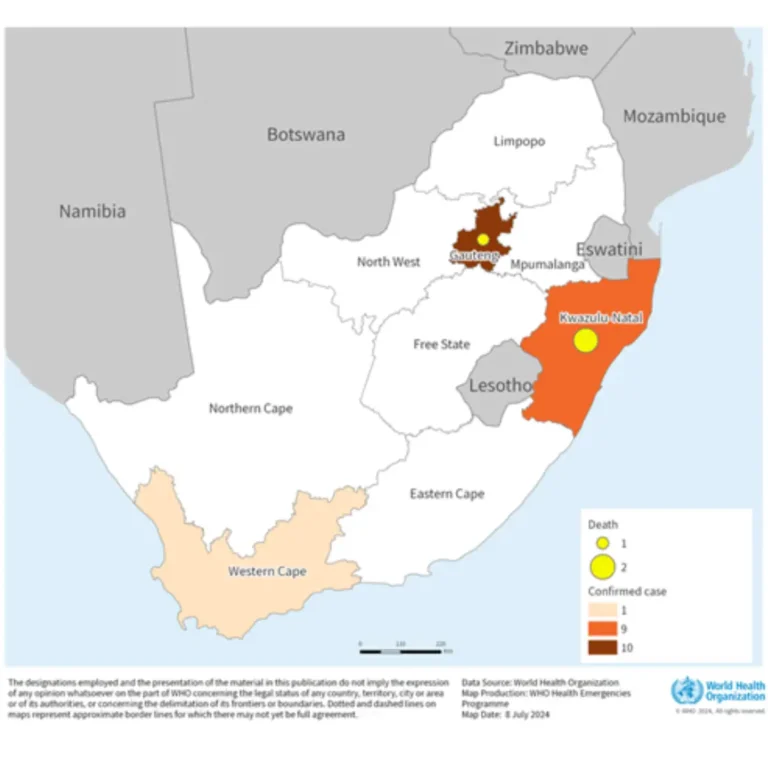
As of 4 August 2024, South Africa has 24 confirmed Mpox cases, including three deaths. These cases were reported in three of nine provinces: Gauteng (12 cases; 1 death), Western Cape (1 case), and KwaZulu-Natal (11 cases; 2 deaths).
Health officials and the National Institute for Communicable Diseases (NICD) have been closely monitoring the situation, providing updates and guidance to the public. Dr. Michelle Groome, head of the NICD’s Division of Public Health Surveillance and Response, emphasised the importance of early detection and isolation to prevent further spread.
How is Mpox Transmitted?
Mpox transmission occurs through various routes:
- Skin-to-skin contact: Direct contact with an infected person’s lesions.
- Respiratory droplets: Prolonged face-to-face exposure to respiratory droplets.
- Bodily fluids: Contact with bodily fluids or contaminated materials.
The virus can be transmitted by pregnant persons to the unborn child
Anyone can get Mpox; however, people with multiple sexual partners are at increased risk. Health officials emphasise contact tracing and preventive measures to control the spread. Simple preventive measures, such as avoiding close contact with infected individuals and practising good hygiene, can significantly reduce the risk of infection.
Mpox Symptoms
Recognising Mpox symptoms early is crucial for timely medical intervention.
Symptoms typically include:
Fever: Often the first symptom, accompanied by chills and sweats.
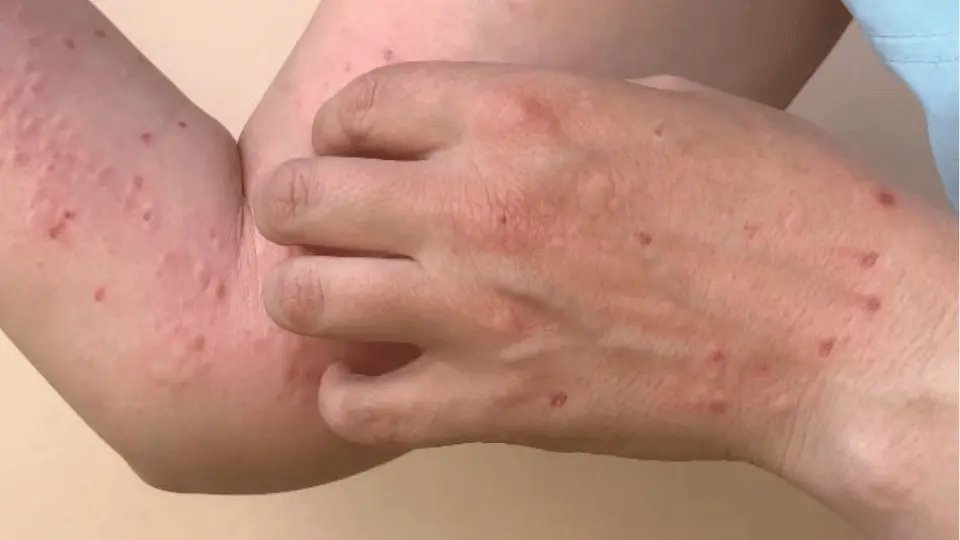
Rash: Develops 1-3 days after the fever, beginning on the face and spreading to other body parts. The rash progresses from macules to pustules before forming a scab and eventually falling off. Visual identification of the rash can aid in early diagnosis and containment.
Swollen lymph nodes: Distinguishing feature from other poxviruses.
Recognising these early symptoms is crucial for prompt isolation and treatment, helping to prevent further transmission.
How to Prevent Mpox
Preventing Mpox involves several practical steps. Avoiding close contact with infected individuals and practising good hygiene, such as regular handwashing, are essential. The Mpox vaccine, which is available in South Africa, offers significant protection. Public health recommendations also stress the importance of following guidelines issued by health authorities and staying informed about the latest developments.
Treatment and Cure
Treatment for Mpox focuses on symptomatic relief and preventing complications, which includes:
At-home care: Managing symptoms with over-the-counter medications for pain relief, rest and maintaining hydration.
Medical treatments: Antiviral drugs and immunoglobulins for severe cases.
Research is ongoing for specific treatments and potential cures. It’s important to seek medical help if symptoms worsen or complications arise with at-home care. Severe cases may require hospitalisation and supportive care.
Addressing Common Questions
Is Mpox dangerous? While Mpox can cause severe illness, it is generally not as deadly as smallpox. The case fatality rate varies, but it is generally lower than that of smallpox.
The Mpox virus can be lethal in some cases, particularly among immunocompromised individuals or those with underlying health conditions. However, with appropriate medical care and supportive treatment, most patients recover fully.
Impact on Public Health
The broader public health implications of the Mpox outbreak are significant. The South African government and healthcare providers have mobilised resources to contain the outbreak and prevent further spread. The World Health Organization (WHO) and other international bodies are also involved, providing support and guidance. Public health campaigns and community outreach programs are essential to educate the public about Mpox and encourage preventive measures.
Conclusion
In conclusion, Mpox is a rare but potentially serious disease that requires public awareness and preventive health care measures to control its spread.
To manage and address Mpox-related concerns, leveraging online doctor consultations can be highly beneficial. Docotela offers convenient and reliable online doctor consultations, allowing individuals to seek medical advice and support without leaving their homes.
Book an online consultation with a doctor to ensure you receive timely and expert medical guidance. Online consultations not only provide ease of access but also help minimise the risk of spreading infections, making them a vital tool in managing public health crises like the Mpox outbreak.
